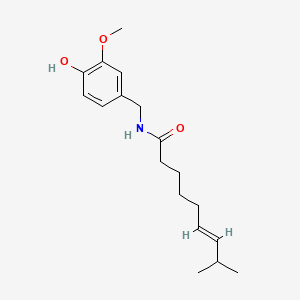
Capsaicin (Figure 1) is the major compound in chili peppers that triggers the reception of “spice”. It acts on the transient receptor potential vanilloid subfamily member 1 receptor, or just TRPV1. The TRPV1 receptor is found across sensory neurons, and because the response is followed by a long refractory period, capsaicin has been applied as a therapeutic to help with pain (Sharma et al. 2013). In recent years, research into the applications of capsaicin has proposed its use as an anti-cancer treatment, but there has also been research that suggests it has carcinogenic properties (Bode and Dong 2011).
The anticancer mechanism of capsaicin has been investigated, proposing that it induces cell-cycle arrest and apoptosis. It has been shown to do so in multiple types of cancer, including liver, pancreatic, colonic, esophageal, skin, leukemia, and more. The exact mechanism requires more research to confirm, but it is speculated that for triggering apoptosis, capsaicin targets proteins involved in the mitochondrial death pathway (Clark and Lee 2016). The mitochondrial death pathway is a major apoptosis pathway which occurs when apoptogenic molecules trigger the outer membrane to dissolve, leading to apoptosis (Gupta et al. 2009). Capsaicin has also been found to enhance the activity of the p53 tumor suppressor. As for cell cycle arrest, it has been shown that capsaicin does so by decreasing levels of vital cyclin-dependent kinases. Additionally, research indicates that capsaicin not only targets cancer on a cellular scale, but has anti-angiogenic and metastatic properties (Clark and Lee 2016).
Research into the chemotherapeutic potential of capsaicin has been accompanied by numerous studies that demonstrate its carcinogenic properties. In many in vivo studies on rats, capsaicin has resulted in cancer growth in the liver and stomach (Bode and Dong 2011). Numerous studies report both the genotoxic and carcinogenic effects of capsaicin, however it is of note that many of the studies done on its carcinogenic potential were not done with pure capsaicin (Bley et al. 2012). A study done in 2004 using pure capsaicin found no increase in mutations in bacterial assay tests, concluding it as not genotoxic (Chanda et al. 2004).
Capsaicin has been shown to be safe and effective in treating pain. Additionally, its potential as a treatment for cancer should not be dismissed as it may have mechanisms which inhibit cancer at multiple stages in its growth and spread. Regardless, more research should be conducted into capsaicins properties due to the great divide of studies confirming it as both a cancer-preventative and cancer-inducing agent.
Bibliography
Bley, Keith, Gary Boorman, Bashir Mohammad, Donald McKenzie, and Sunita Babbar. 2012. “A Comprehensive Review of the Carcinogenic and Anticarcinogenic Potential of Capsaicin.” Toxicologic Pathology 40 (6): 847–73. https://doi.org/10.1177/0192623312444471.
Bode, Ann M., and Zigang Dong. 2011. “The Two Faces of Capsaicin.” Cancer Research 71 (8): 2809–14. https://doi.org/10.1158/0008-5472.CAN-10-3756.
Chanda, Sanjay, Greg Erexson, Colin Riach, et al. 2004. “Genotoxicity Studies with Pure Trans-Capsaicin.” Mutation Research/Genetic Toxicology and Environmental Mutagenesis 557 (1): 85–97. https://doi.org/10.1016/j.mrgentox.2003.10.001.
Clark, Ruth, and Seong-Ho Lee. 2016. “Anticancer Properties of Capsaicin Against Human Cancer.” Review. Anticancer Research 36 (3): 837–43.
Gupta, Sanjeev, George EN Kass, Eva Szegezdi, and Bertrand Joseph. 2009. “The Mitochondrial Death Pathway: A Promising Therapeutic Target in Diseases.” Journal of Cellular and Molecular Medicine 13 (6): 1004–33. https://doi.org/10.1111/j.1582-4934.2009.00697.x.
PubChem. 2005. “Capsaicin.” https://pubchem.ncbi.nlm.nih.gov/compound/1548943.
Sharma, Surinder Kumar, Amarjit Singh Vij, and Mohit Sharma. 2013. “Mechanisms and Clinical Uses of Capsaicin.” European Journal of Pharmacology 720 (1): 55–62. https://doi.org/10.1016/j.ejphar.2013.10.053.
Leave a Reply
You must be logged in to post a comment.