Those moments when you are famished, but have an untouched assignment due in three hours, a $10 fast-food combo feels like the only choice. It is quick, filling, and it doesn’t wreck your wallet, at least not in the moment. The initial fee is only the sticker price; the true cost is reflected in healthcare spending and missed workdays, increasing group and personal spending, which will be explained in this post through an economic, public health, and biological perspective.
Ultra-processed foods are products that appear efficient in the short term because they are engineered to be cheap, shelf-stable, and convenient, and aggressively marketed. The issue is that markets don’t automatically price in the downstream costs of a widespread poor diet. This process is called externalities: costs created by a product that aren’t included in the price tag, like higher healthcare spending and lower productivity linked to diet-related disease. When diet-driven conditions scale across a population, the burden becomes measurable at the national and global level, and it stops being just an “individual choice” problem (Swinburn et al., 2019).
The bigger question is what happens when an entire food environment nudges people toward ultra-processed eating patterns every day. Large cohort studies have found that higher intake of ultra-processed foods is associated with a higher risk of all-cause mortality (Campà et al., 2019). However, observational studies can’t prove causation on their own, these patterns matter because they show up across large groups over time and can help guide prevention strategies. Public health also focuses on how harms don’t fall evenly: time pressure, limited access to fresh foods, and targeted marketing can make “cheap calories” the default option in some communities, widening health inequities (Monteiro et al., 2019).
In a tightly controlled inpatient randomized trial, participants ate about 500 more calories per day on an ultra-processed diet than on an unprocessed diet, even when meals were designed to be similar in presented calories and key nutrients (Figure 1). That suggests the difference isn’t just willpower, but rather texture, eating rate, and satiety signalling can shift how much we consume (Hall et al., 2019). Over time, frequent spikes in refined carbs and fats can push metabolism toward insulin resistance and inflammation, while diet patterns can also reshape the gut microbiome in ways linked to metabolic disease (Zinöcker & Lindseth, 2018). Highly processed foods are also more likely to be described as “hard to stop eating,” which matters because habits form around what feels rewarding fast (Schulte et al., 2015).
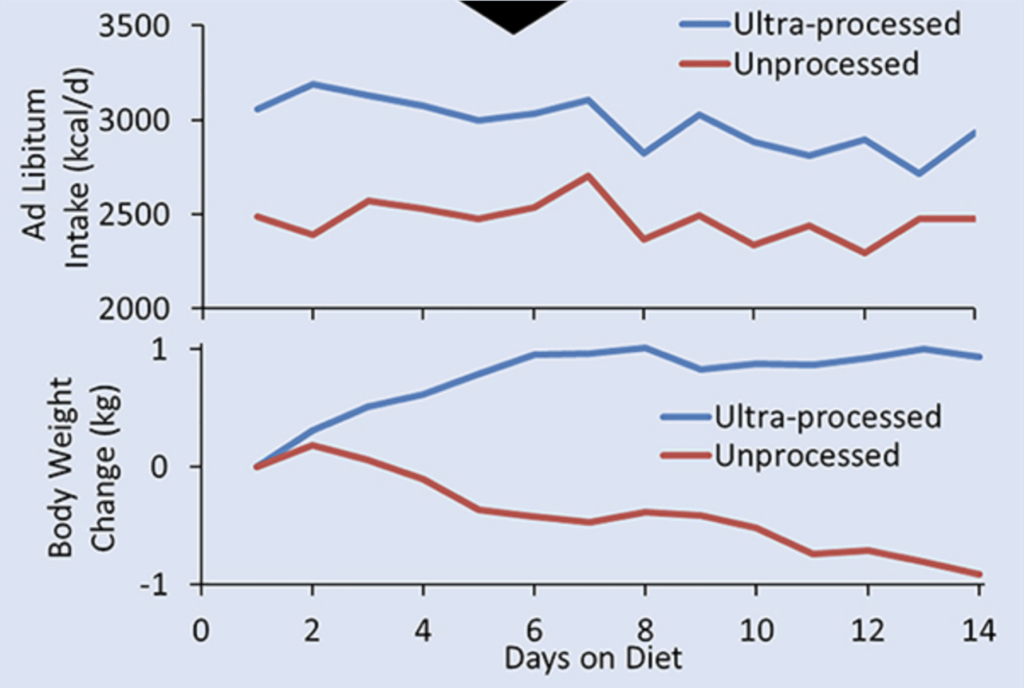
The ultra-processed diet consistently consumed 500 extra calories per day compared to the recommended calorie intake. This resulted in higher triglyceride levels in adipose tissue, increasing fat tissue’s release of signalling molecules that promote low-grade inflammation, which is why weight gain is linked to a higher risk of chronic disease. Furthermore, cells can become less responsive to insulin, leading to insulin resistance and, eventually, an increased risk of type 2 diabetes. The figure shows a short-term version of a long-term problem: if ultra-processed eating makes you take in more energy without feeling fuller, your metabolism shifts toward constantly needing more calories for everyday functions (Hall et al., 2019).
The next time a fast-food meal feels like a bargain, it is worth remembering the bigger equation: low price now can mean higher cost later. If we want cheap food to actually be cheap in the long run, the solution can’t only be personal discipline; it has to include smarter environments, better access, and policies that make the healthier choice the easier choice.
Work Cited:
Hall, Kevin D., Alexis Ayuketah, Robert Brychta, et al. 2019. “Ultra-Processed Diets Cause Excess Calorie Intake and Weight Gain: An Inpatient Randomized Controlled Trial of Ad Libitum Food Intake.” Cell Metabolism 30 (1): 67-77.e3. https://doi.org/10.1016/j.cmet.2019.05.008.
Monteiro, Carlos A., Geoffrey Cannon, Renata B. Levy, et al. 2019. “Ultra-Processed Foods: What They Are and How to Identify Them.” Public Health Nutrition 22 (5): 936–41. https://doi.org/10.1017/S1368980018003762.
Rico-Campà, Anaïs, Miguel A. Martínez-González, Ismael Alvarez-Alvarez, et al. 2019. “Association between Consumption of Ultra-Processed Foods and All Cause Mortality: SUN Prospective Cohort Study.” BMJ, May 29, l1949. https://doi.org/10.1136/bmj.l1949.
Schulte, Erica M., Nicole M. Avena, and Ashley N. Gearhardt. 2015. “Which Foods May Be Addictive? The Roles of Processing, Fat Content, and Glycemic Load.” PLOS ONE 10 (2): e0117959. https://doi.org/10.1371/journal.pone.0117959.
Swinburn, Boyd A., Vivica I. Kraak, Steven Allender, et al. 2019. “The Global Syndemic of Obesity, Undernutrition, and Climate Change: The Lancet Commission Report.” The Lancet 393 (10173): 791–846. https://doi.org/10.1016/S0140-6736(18)32822-8.
Zinöcker, Marit, and Inge Lindseth. 2018. “The Western Diet–Microbiome-Host Interaction and Its Role in Metabolic Disease.” Nutrients 10 (3): 365. https://doi.org/10.3390/nu10030365.
Leave a Reply
You must be logged in to post a comment.