Imagine if scientists could test hundreds of drugs on a virtual version of your body before you ever took a single pill. Instead of relying entirely on trial-and-error in clinical trials, researchers could simulate treatments on a personalized digital model of a patient. This emerging technology, known as a digital twin, is rapidly gaining attention as a potential tool to transform human health.
The concept of digital twins originated in the 1960s, when NASA developed virtual models of spacecraft systems to monitor performance and simulate failures during missions such as Apollo 13 (Katsoulakis et al. 2024), and has since evolved into a powerful tool in healthcare. A digital twin is a dynamic virtual representation of a real-world system that continuously updates using real-time data (Katsoulakis et al. 2024). In medicine, this involves constructing a computational model of an individual patient by integrating biological, environmental, and clinical information, contributing to the emergence of precision medicine, an approach to disease treatment and prevention that accounts for individual variability in genes, environment, and lifestyle (Figure 1). Unlike traditional models, digital twins evolve as new data are collected and can incorporate diverse sources such as genetic sequencing, medical records, wearable devices, environmental exposures, and patient-reported information (De Demenco et al. 2025). By integrating these datasets, researchers can simulate disease progression, predict patient responses to treatments, and explore potential health trajectories before interventions are applied in real-world clinical settings.
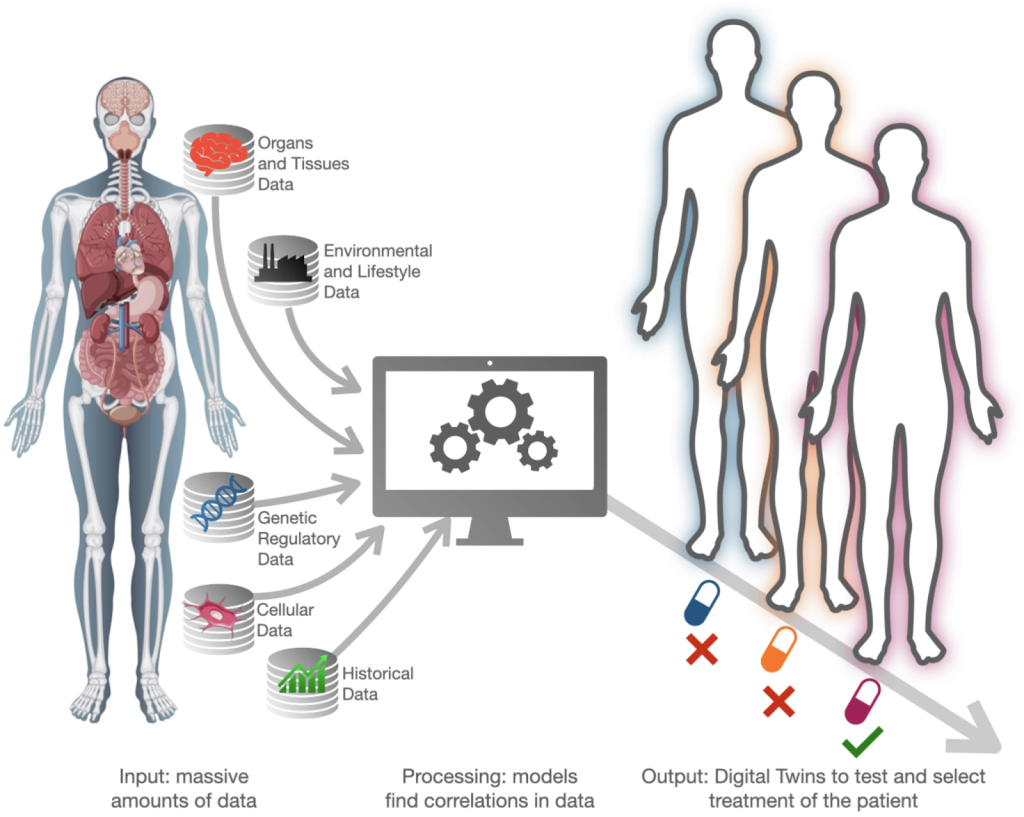
In medical contexts, digital twins link the physical patient, a computational model representing their biology, and continuous data exchange between the two systems (Mekki et al. 2025). As new data are integrated, the virtual model updates in near real time, allowing clinicians to simulate how organs respond to treatments, predict complications, and support medical decision-making. Beyond clinical care, digital twins also play a growing role in precision medicine, where treatments are tailored to individual patients rather than generalized populations. These models can simulate how a specific patient may respond to drugs or interventions, allowing clinicians to test therapeutic strategies virtually before applying them in practice (De Domenico et al. 2025). One promising application of digital twins lies in drug discovery, an area of biomedical research that is both expensive and time-consuming. Digital twins could improve this process by allowing researchers to simulate biochemical interactions, predict drug targets, and test therapies virtually before human trials begin (Katsoulakis et al. 2024).
However, this technology also raises significant ethical concerns. Since digital twins rely on large volumes of sensitive health data, including genetic information, medical histories, and real-time physiological monitoring, issues surrounding privacy, data security, and informed consent become especially complex (Huang et al. 2022). Patients may not fully understand how their data are collected, shared, or reused across platforms, raising questions about ownership and control over personal health information. In addition, the use of large, heterogeneous datasets introduces the risk of algorithmic bias, particularly if certain populations are underrepresented in training data. This could lead to unequal or less accurate predictions for marginalized groups, potentially reinforcing existing health disparities. Lastly, the increasing reliance on predictive models may shift the doctor–patient relationship, raising questions about trust, autonomy, and the role of human judgment in care. Addressing these ethical challenges through transparent data governance, inclusive model design, and clear regulatory frameworks will be essential as digital twins move closer to widespread clinical implementation.
By combining biology, artificial intelligence, and computational modeling, digital twins offer the potential to transform healthcare, enabling safer treatments, accelerating drug development, and advancing personalized care. At the same time, realizing this potential will require careful attention to the ethical, social, and institutional challenges that accompany such a powerful and data-driven approach to medicine.
References:
De Domenico, Manlio, Luca Allegri, Guido Caldarelli, et al. 2025. “Challenges and Opportunities for Digital Twins in Precision Medicine from a Complex Systems Perspective.” Npj Digital Medicine 8 (1): 37. https://doi.org/10.1038/s41746-024-01402-3.
Huang, Pei-hua, Ki-hun Kim, and Maartje Schermer. 2022. “Ethical Issues of Digital Twins for Personalized Health Care Service: Preliminary Mapping Study.” Journal of Medical Internet Research 24 (1): e33081. https://doi.org/10.2196/33081.
Katsoulakis, Evangelia, Qi Wang, Huanmei Wu, et al. 2024. “Digital Twins for Health: A Scoping Review.” Npj Digital Medicine 7 (1): 77. https://doi.org/10.1038/s41746-024-01073-0.
Mekki, Yosra Magdi, Gijs Luijten, Elisabet Hagert, et al. 2025. “Digital Twins for the Era of Personalized Surgery.” Npj Digital Medicine 8 (1): 283. https://doi.org/10.1038/s41746-025-01575-5.
Leave a Reply
You must be logged in to post a comment.